THE VALUE OF CT ANGIOGRAPHY (CTA) IN COMPREHENSIVE EVALUATION OF VASCULAR DISEASE AFTER ULTRASOUND SCREENING
5/12/2026 11:33:56 AM
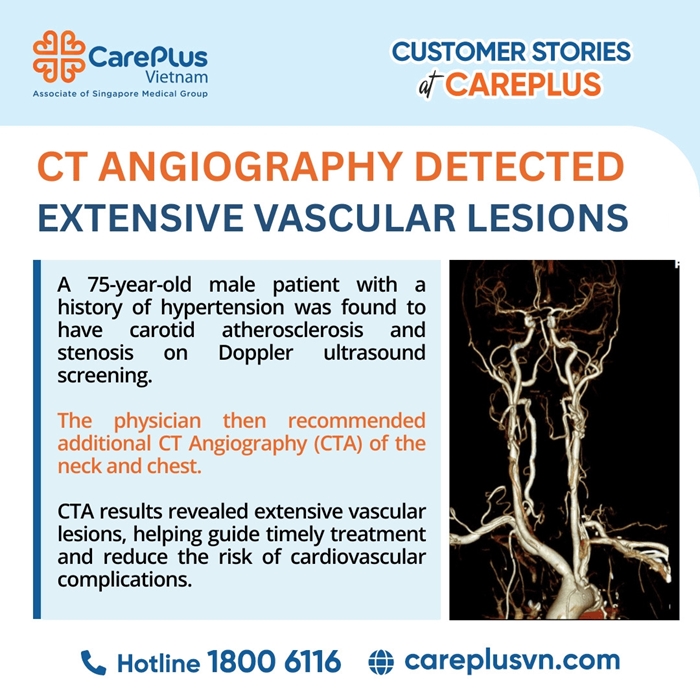
A 75-year-old male patient with a long history of hypertension and high cardiovascular risk underwent routine carotid Doppler ultrasound screening. The examination revealed atherosclerotic plaques and stenosis in portions of the carotid arterial system. However, due to the physical limitations of ultrasound waves, structures located deep within the thorax (such as the aortic arch) or intracranial vessels could not be adequately assessed.
Given the suspicion of multi-vessel atherosclerotic disease, the clinical team decided to further evaluate the patient with CT Angiography (CTA) of the neck and chest.
CTA IMAGING FINDINGS
CTA not only confirmed the lesions identified on ultrasound but also detected additional serious vascular abnormalities in anatomical regions inaccessible to ultrasound imaging.
Thoracic Aortic Arch
Calcified atherosclerosis with a penetrating atherosclerotic ulcer (PAU) located along the outer wall of the aortic arch
Lesion size: 6.5 × 4 mm
Right Carotid–Vertebral Arterial System
Severe stenosis (~80%) of the proximal right internal carotid artery (ICA) caused by calcified atherosclerotic plaque
Measured according to NASCET criteria
Left Carotid–Vertebral Arterial System
Ulcerated atherosclerotic plaque in the left common carotid artery (CCA)
Ulcer size: 3 × 2 mm
Approximately 50% stenosis at the origin of the left subclavian artery
Severe (~80%) stenosis of the left vertebral artery (V2 segment), measured according to ESCT criteria
PROFESSIONAL ANALYSIS
The use of CTA in this case provided critical diagnostic value and significantly changed the clinical management strategy.
1. Eliminating Anatomical “Blind Spots” – Detecting Life-Threatening Lesions
The most significant finding was the penetrating atherosclerotic ulcer (PAU) in the thoracic aortic arch.
PAU is classified as a form of Acute Aortic Syndrome (AAS), occurring when an atherosclerotic plaque erodes through the intimal layer and penetrates into the medial layer of the aortic wall. The “mushroom-shaped” morphology suggested progressive deep wall involvement.
If evaluation had stopped at carotid ultrasound alone, this lesion would almost certainly have been missed.
The patient could have faced catastrophic complications such as aortic dissection or aneurysmal rupture, both associated with extremely high mortality rates.
Impact on Treatment Strategy
Thanks to CTA findings, the patient was immediately placed under:
- strict blood pressure monitoring,
- scheduled imaging follow-up,
- multidisciplinary consultation with thoracic vascular specialists to consider future endovascular intervention if indicated.
2. Accurate Assessment of Stenosis Severity
CTA enables precise three-dimensional measurement of vascular stenosis using internationally accepted standards (NASCET/ESCT).
Imaging demonstrated:
- severe (80%) stenosis of the right internal carotid artery,
- severe (80%) stenosis of the left vertebral artery.
Clinical Significance
Severe carotid artery stenosis is a major risk factor for ischemic stroke due to embolic events or reduced cerebral perfusion.
Clinical symptoms and imaging findings must be correlated to determine the need for revascularization procedures such as:
- Carotid Endarterectomy (CEA)
- Carotid Artery Stenting (CAS)
For vertebral artery stenosis, aggressive medical management is typically prioritized, while endovascular intervention is reserved for patients with refractory vertebrobasilar insufficiency symptoms.
3. Plaque Characterization and Embolic Risk Evaluation
CTA’s high spatial resolution allowed detection of a small ulceration (3 × 2 mm) within the atherosclerotic plaque of the left common carotid artery.
Ulcerated plaques are considered:
👉 unstable atherosclerotic plaques.
These ulcerated surfaces are highly thrombogenic and may lead to cerebral infarction through embolic mechanisms.
This imaging finding directly influenced the optimization of:
- antiplatelet therapy,
- intensive lipid-lowering treatment.
CLINICAL VALUE OF CTA
Doppler ultrasound remains an excellent first-line screening tool because it is:
- safe,
- non-invasive,
- cost-effective,
- widely available
However, when ultrasound reveals vascular atherosclerosis or stenosis in high cardiovascular-risk patients, CTA becomes an essential next step.
CTA provides a comprehensive “vascular roadmap” extending:
- from the thoracic aortic arch
- through the carotid and vertebral arteries
- to the intracranial circulation and Circle of Willis.
The combination of Doppler ultrasound and CTA helps clinicians:
- avoid missing deep vascular lesions,
- accurately stratify stroke risk,
- personalize treatment strategies,
- determine whether medical therapy or surgical/endovascular intervention is more appropriate.